Quick Facts
- In some cases, scar tissue formation can be excessive.
- The two types of excessive scar tissue formation are known as keloid and hypertrophic scarring.
- Keloid scarring tends to overgrow the boundary of the initial injury, and can be painful and/or itchy. Keloids usually don’t get better with time. Surgical revision of keloid scars can make them worse.
- Hypertrophic scarring tends to remain within the boundary of the initial injury, and get better with time.
- Darker skin types predispose to keloid scar formation.
- Keloid and hypertrophic scars can be treated with a combination of fractional carbon dioxide laser and cortisone applied topically.
For the treatment of atrophic (indented) acne scars, please see our acne scarring page.
What are keloid and hypertrophic scars?
Scar formation can be a normal part of the tissue healing process. In some cases, scar formation can be excessive beyond what is necessary to heal a wound. Keloid and hypertrophic scars result from an abnormal wound healing response in particular individuals. They are the body’s response to trauma, inflammation, surgery or burns, and sometimes can occur spontaneously. Common skin injuries that lead to keloid growth are; surgery, ear piercing, lacerations, abrasions, tattooing, vaccinations, injections, insect bites, burns, acne, chicken pox, folliculitis/ingrown hairs, and shingles. Their appearance is of a raised, often red/purple coloured scar that can have a firm consistency.
The difference between keloid and hypertrophic scars is difficult to determine at times. Keloid scars tend to extend from the boundary of the original wound and do not regress, whereas hypertrophic scars tend to not extend from the original would and regress over time.
For more general information on scarring, click here.
Table: Differences between keloid and hypertrophic scarring
|
Hypertrophic scars |
Keloid scars |
|
Develop soon after injury |
May have delayed development after injury |
|
Subside with time |
Rarely subside with time |
|
Limited boundary |
Overgrows wound boundary |
|
Size proportional to injury |
Minor injury may produce a large scar |
|
Occurs across areas of motion/tension |
Occurs in any areas |
| Not usually painful or itchy | Can be painful or itchy |
|
Improve with surgery |
Often worsened by surgery |
What factors predispose to keloid or hypertrophic scarring?
Keloid and hypertrophic scarring is more common in darker skin. Hypertrophic scarring is more common than keloid scarring.
Increased skin tension or wound tension can also predispose to hypertrophic and keloid scarring. Keloids tend to develop more readily after puberty, and are more common in younger individuals rather than older individuals due to the greater tension of younger skin that predisposes to increased scarring.
Darker parts of the skin are more predisposed to keloid or hypertrophic scarring, thus the palms and soles of feet are rare places for keloids to form.
How can I treat hypertrophic and keloid scarring?
One of the key methods we utilise for treating keloid and hypertrophic scars is our fractional co2 laser combined with topical cortisone. Cortisone is often injected into scars, however, this can cause skin or fat atrophy which leads to indentations or divots in the area injected. Cortisone acts by stopping excess collagen production that causes scar tissue formation.
Instead of direct injection of cortisone, fractional CO2 laser is used to create channels in the skin followed by topical cortisone application. This allows cortisone to penetrate evenly into the skin. Furthermore, fractional CO2 lasers re-organise the collagen fibres in scars to help smooth and flatten particular types of scars. This combination of fractional CO2 and cortisone is effective for keloid, hypertrophic and burn scars.
Other traditional methods of scar treatment are listed as follows;
Cryotherapy – this involves the application of liquid nitrogen (commonly known as dry ice) to the keloid scar. Clinical studies have shown flattening within a few sessions. This can be combined with corticosteroid injections into the scar.
Corticosteroids – Corticosteroid creams and injections (including triamcinolone acetonide) are a common treatment modality for keloid scarring. Although, they do not make keloids disappear, they can help to flatten and provide symptomatic relief. A series of injections is usually required to gain the maximal effect – usually at 2 – 3 week intervals.
5-Flurouracil injections (5-FU) – can also be used alone or in combination with corticosteroid injections into keloid scars. This treatment stops fibroblasts from making new scar tissue. 5-FU is also used as a chemotherapy agent normally.
Surgery – surgical excision of a keloid scar is commonly ineffective as the recurrence rate is very high. Combining surgery with corticosteroid injections and/or external pressure can help reduce the recurrence rate. Surgery alone is generally not the treatment of choice with the majority of keloid scars. However, for some keloid scars, such as the ones that occur on earlobes, may require surgical excision due to their large size combined with medical therapy. Hypertrophic scars, conversely, do not tend to recur with surgery, and sometimes surgical excision of hypertrophic scars can be successful if done in a manner which is conducive to healing. Usually this requires the scar to be excised and resutured so that there is minimal tension on the wound edges and they oppose well. This requires the incisions to be made a particular direction of the skin where the tension is less in that direction.
Laser treatment – Pulsed dye lasers can be used to help remove the redness from keloid scars. They are attracted to the haemoglobin (blood) in the scars and can help to shut down the blood vessels supplying the scar and reduce the redness in the scar.
Topical silicone gel – Topical silicone gel sheeting is a new and painless method to treat hypertrophic and keloid scars. Although the actual mode of action is unknown, it is hypothesised that it could be due to hydration of the skin from the silicone stimulates new collagen production. Usually treatment can commence once the skin is healed over (no open wounds), and that 2 months of wear is adequate for the prevention and treatment of hypertrophic and keloid scars. Examples of silicone gels include Dermatix.
Pressure garments – are particularly useful to help prevent scarring after burns. Collagen maturation is hastened and the scar flattens. The garments must however be worn for at least 9 months day and night in order to prevent the scars from forming, as well as be tight enough to provide adequate pressure.
Radiation therapy – In a similar manner to radiotherapy treatment for various cancers, radiation therapy can help to reduce scar tissue formation in keloid scars.
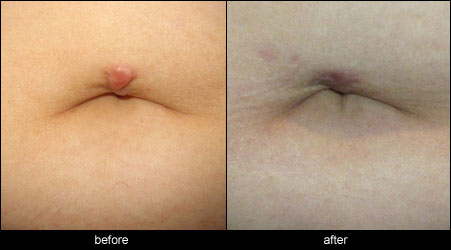
Case study
This is a female who had a belly button piercing that caused keloid scarring. The treatment shows the result three months after one injection with triamcinolone (corticosteroid injection).
Why should I choose The Victorian Cosmetic Institute to treat my hypertrophic/keloid scars?
At The Victorian Cosmetic Institute, we have cosmetic physicians that will be able to look at non-surgical (including laser) treatment of scars. The first step is simply contacting us. We will then discuss with you what is a realistic and achievable outcome, and what to expect from your scar treatment.
Making that first phone call about any cosmetic procedure can be a confronting task – many of our patients have preferred filling out our online enquiry form. We can then contact you with an understanding of the results you are hopeful of achieving and ensure the treatment is appropriate. It’s as easy as clicking either of the buttons below and completing the provided form.
Otherwise, you can phone us directly on 1300 863 824.